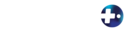Stimulants and survival: Unhoused Coloradans turn to methamphetamine as a form of protection
COLORADO SPRINGS, Colo. — Stephen Copeland hardly knows life outside of prison.
He has spent 24 of his 65 years of life rotating through correctional facilities in the state. He can count them all and recite how long he stayed in each, and for what offense.
Most recently, Copeland did 24 years in the Limon Correctional Facility for arson.
Now living on the street in Colorado Springs, Copeland does his best to stay out of trouble by cleaning up after himself, not using drugs in front of too many people and avoiding fights. But life inside could have been worse, Copeland said. He spent his days lifting weights, socializing and trying to forget the grim realities of living inside a locked box with little to look forward to on the outside.
Other prisoners could be brutal, he said. Fights were frequent and Copeland said inmates often had to make rash decisions to protect themselves or others.
He survived as a member of the Aryan Brotherhood, a white supremacist gang. He was a member of Aryan Brotherhood long before prison, though Copeland said people have two choices when they're incarcerated: join a gang or fall victim to a gang.
“I got more respect in prison than I did out here, by far,” Copeland said. “I knew all the fellows in the joint and they all knew me.”
Copeland was introduced to white supremacy as a teenager in Colorado Springs, where he grew up. He said the Aryan Brotherhood and its beliefs aren’t uncommon in Colorado’s second-largest city. On its surface, Colorado Springs is known for its proximity to Pikes Peak, military presence and its evangelical base. But the city has a dark underbelly, Copeland said. One of white supremacy, violence and heavy drug usage.
Around the same time he was introduced to violent racism, Copeland also found methamphetamine. He snorted and ingested the drug for decades, then began smoking it after his most recent exit from prison, six years ago.
Copeland is part of a growing number of people experiencing homelessness who use methamphetimine to stay awake longer and protect their belongings. While opioids used to be responsible for the majority of overdose deaths, El Paso County data show meth is now to blame for the majority share of overdoses in the Colorado Springs area.
Related Stories
In the early years of his usage, sobriety was a nice idea, Copeland said. Though it may never have been a real possibility, it was always a goal in the distant background.
At 65, all of Copeland’s family members are dead, he has no close friends, and his days revolve around evading police and staying awake long enough to guard his belongings from other unhoused people who are seeking replacements after police take their belongings. Copeland also has Crohn’s disease, a digestive disease that makes eating difficult and often painful. He described the disease flare-ups as “you’re starving but you can’t eat because you’ll get sick.”
Denim shorts that stop just above his kneecaps reveal sores up and down Copeland’s legs. They are symptoms of the disease. He doesn’t wear a shirt, exposing more sores and bones on the upper half of his body covered by thin layers of skin.
On an April morning, he smokes a cigarette next to a group of other unhoused folks on a torn-up couch at the corner of Uintah and 19th Streets, just outside a shopping plaza with a grocery store, car wash and thrift store. The group discusses a path forward after police took an acquaintance's sleeping bag, tent and clothing. Copeland’s belongings survived the raid. He’s not sure how, but he’s grateful.
The day is standard for Copeland: try and force himself to eat some of what he bought with his monthly $60 in food stamps, cross his fingers that the police don’t target his belongings and smoke enough meth to make life a little more bearable.
For Copeland, life without meth sounds far worse than one with it.
“Right now, reality sucks and meth is an escape from reality,” Copeland said. “I used to have pretty good control over my use, but now I don’t care anymore.”

Steven Copeland holds up his pipe to show his primary method of using meth. Copeland says he uses more meth now than ever before, calling it an effective painkiller for chronic health issues and also an escape from the challenges of homelessness.
“Meth: you can’t get away from it”
Though Copeland has few people he considers “friends,” he says he knows most unhoused people in Colorado Springs, at least those within two miles of him.
“Pretty much all of them do meth,” Copeland said of others living outside. “This is probably the meth capital of the United States. It’s everywhere. You can’t get away from it.”
Copeland said he has a few friends with indoor housing, and he occasionally exchanges drugs for a few-night’s stay. A gram of meth and an eighth of weed can buy him three nights, a few home-cooked meals and a shower. While living on the streets and forcing himself to eat dry noodles, a meal and shower are luxurious for Copeland.
The 2022 Point-in-Time Count, a survey administered annually in El Paso County measuring the county’s houseless population and factors contributing to homelessness, found 14% of unhoused people in Colorado Springs cite Substance use disorder as a reason for their homelessness.
PJ Higgins, the opioid prevention project manager for the Community Health Partnership, a Colorado Springs nonprofit that works on health equity issues, said that number doesn’t represent everyone who has substance use disorder. Most who have the disorder are not homeless, and many who are experiencing homelessness use substances but don’t cite their usage as a reason for their circumstances.
“Certainly, there’s a strong interaction between people who are homeless and substance use disorder,” Higgins said. “Substance Use Disorder does become a significant barrier to exiting homelessness.”
Homeless shelters do not allow drugs inside their facilities, and many pathways to long-term housing require sobriety as a prerequisite. Those who are ready to get sober immediately can choose rehabilitation facilities, but those are often expensive. And for many, sobriety is an ultimate goal, but the harsh realities of living outside make it feel impossible.
“When people don’t have access to care, often what happens is they turn to a substance in order to help navigate or self-medicate the condition they’re dealing with,” Higgins added. “Thinking about Substance Use Disorder not as a series of bad choices but as the result of a need to manage trauma and its impacts on mental health and state of mind and ability to navigate the ups and downs in life in a way that’s healthy is a key component of understanding.”

Melissa Chizmar is the prevention services manager at Southern Colorado Health Network, where she oversees the safe needle and supplies exchange program.
Melissa Chizmar, prevention services manager at the Southern Colorado Health Network, said of the unhoused folks she works with, more than half use methamphetamine.
“Meth, because it’s a stimulant, is going to keep people awake,” Chizmar said. “I think that’s important when you think about how cold winter nights can be and the thefts you see during that time because of exposure, which can certainly be a reason why some people might use meth, to ensure they survive the night.”
Meth and heroin are the most used substances reported among the unhoused community, Chizmar said. Meth is the most common.
Many unhoused people, Chizmar explained, turn to meth and other substances to cope with trauma – either pre-existing trauma or trauma made worse by surviving harsh winters and police brutality, realities that come alongside homelessness.
“We definitely see here in Colorado Springs that addiction and homelessness often overlap,” Chizmar said. “Addiction doesn’t occur in a vacuum. It’s often a result of the environment.”
Death in small doses
Until about five years ago, opioids accounted for the majority of drug overdoses, according to the Center for Disease Control and Prevention.
But according to data from the El Paso County Coroner’s Office, methamphetamine accounted for 48 of the county’s 216 drug overdoses in 2022. A combination of meth and fentanyl came just behind with 42 deaths. Fentanyl alone accounted for 36 deaths.
Data provided by the El Paso County Coroner’s Office
Drug-related accidental deaths also jumped by 55% between 2021 and 2022, according to the coroner’s data.
Fentanyl is a powerful opioid used in hospitals as a pain reliever. But the drug – which is 50 times stronger than heroin and 100 times stronger than morphine – is found in much of the drug supply on the streets, often unbeknownst to the people buying and using illicit drugs. Because fentanyl is so potent, two milligrams is considered a lethal dose, according to the United States Drug Enforcement Administration.
Chizmar said many who died via fentanyl overdose often had no idea they were using the potent opioid to begin with. Many thought they were using meth alone without knowing their stimulant was laced with fentanyl. Chizmar described this scenario as extremely common.
“We know that so much supply is contaminated with fentanyl that it’s essentially turning people into poly-substance users, even if that isn’t something they wanted,” Chizmar said.
Though Chizmar and Higgins said fentanyl is difficult to avoid if a person is using illicit drugs, some unhoused folks said the powerful, often lethal opioid is banned from their communities.
“If anybody caught you with it over here, you could get beat up on sight,” said Skittles, a houseless man living on the west side of Colorado Springs. “There’s a certain look with heroin and a certain look with fentanyl. I can tell the difference and fentanyl isn’t allowed.”
Skittles has lived on the streets, off and on, since he was about 12 years old. There aren’t many drugs he hasn’t tried. Though fentanyl and heroin can look similar, Skittles said he can differentiate easily from his decades of personal drug usage. He’s lost friends to fentanyl overdoses and recently revived a friend experiencing an overdose using naloxone, an overdose-reversing nasal spray.
“It was very scary because he didn't even turn blue for a while. No warning, and by the time he turned blue, I’m sure he would have been dead and there would be no bringing him back if I didn’t know what to do,” Skittles said. “It doesn't take much of that fentanyl sh— to kill somebody.”
The worst part, Skittles said, was the friend had no idea he was using fentanyl.
“It’s like playing Russian Roulette with five bullets,” Skittles said. “It’s unlike anything I’ve ever seen.”
After the friend was revived, Skittles told his friend that he needs to get fentanyl testing strips — available at most pharmacies and community health centers — as well as start carrying naloxone.
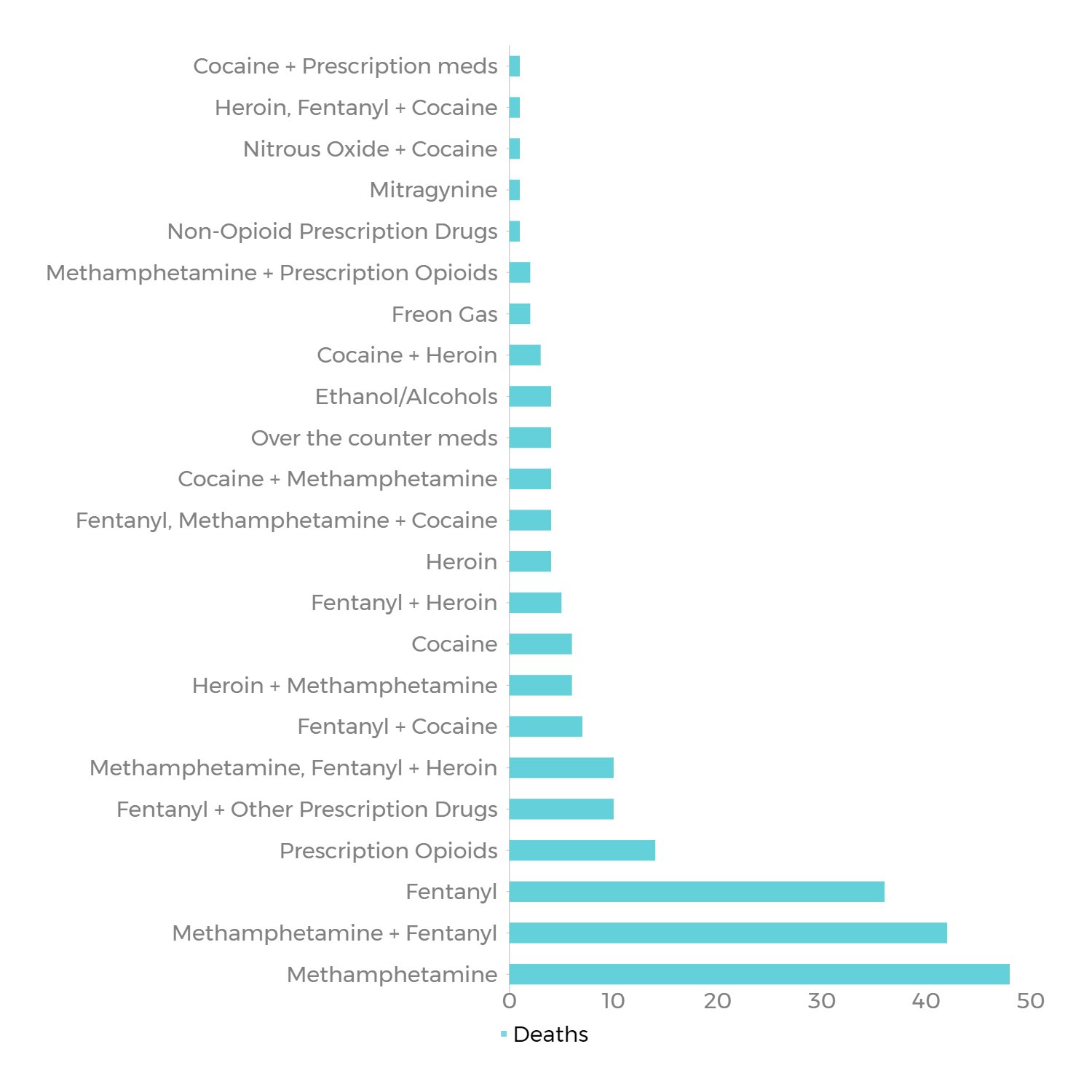
Along with clean supplies for drug use, Southern Colorado Health network provides a variety of health and hygiene products, as well as emergency supplies like naloxone in case of overdoses.
“I was like, look, dude, you’re gonna die if this happens again,” Skittles recalled, clenching a feast and staring straight ahead. “This s– is very, very bad.”
Skittles was an alcoholic for 20 years. He spends most days chasing benzodiazepines with a bottle of Kentucky Deluxe Whiskey. The combination helped him sleep through frosty winter nights and took his mind away from flashbacks of an abusive childhood.
He had enough one day.
“I just got tired of it, honestly,” Skittles said. “Just kind of happened.”
Losing friends to fentanyl and COVID-19 is common for those outside, added Jimbo, another unhoused person and one of Skittles’ friends.
“Being out here is backward,” Jimbo said. “Right is wrong and wrong is right. All your friends are dying off and you just have to keep going.”
Now, Skittles drinks alcohol on occasion and smokes cannabis to make it through his days.
He keeps a sandwich bag of weed in a jar of peanut butter. A half-ripped-off label reveals the crystalized green nuggets. He points to cannabis as a lifesaver for him and those around him.
“I’ve seen a lot of hard s— and I know what it can do, and it isn’t good,” Skittles said.
“But these days, all I want to do is hurt a cheeseburger,” he adds, cracking a half-smile and nodding his head. “Loving and hurting a cheeseburger. That’s it for me.”
Approaching solutions
Higgins and Chizmar said the war-on-drugs methods of criminalizing addiction are ineffective and often cause more harm than good, as they drive people to use illicit substances without knowing what is actually in their supply.
“We know that recovery, over the long-term, is something that’s oriented around building community and connection and finding some way to feel fulfilled and have direction,” Higgins said. “It’s difficult to do that in prison.”
Higgins said Colorado Springs needs more non-criminalization resources across the spectrum of usage, from sober living facilities, detoxification centers and simple harm reduction methods like naloxone and fentanyl test trip accessibility.
“I think there’s a lot more to treatment in terms of how we meet people where they are at,” Higgins said. “Mandated treatment tends to not be as successful as treatment that participated in on a voluntary basis.”
Though such programs have been criticized as “enabling” illicit drug usage, research does not support this. Chizmar also said clean needle access and places to safely dispose of needles is vital. Such access helps prevent the spread of diseases which can often be terminal.
“This has been an incredibly important intervention because it’s extremely effective and there’s over 30 years of research that demonstrates that,” Chizmar said. “It’s primarily a disease prevention model.”
Alison Berg is a journalist at Rocky Mountain PBS. You can reach her at alisonberg@rmpbs.org.
Zach Ben-Amots is an investigative multimedia journalist at Rocky Mountain PBS. You can reach him at zachben-amots@rmpbs.org.